
Position
Associate Professor, Department of Medicine, McGill University
Inaugural Director, McGill Research Centre for Cannabis (2019-2025)
Currently accepting graduate students
Tobacco Product Research Program
The World Health Organization (WHO) estimates that 9 out of 10 people worldwide breathe polluted air- this includes you. This pollution can come from a wide variety of sources, including air pollution caused by industries, traffic (think about all those cars, buses and trucks on the road) and even indoor cooking. In essence, breathing polluted air day-in and day-out can cause heart disease, many types of cancer and chronic lung diseases. Other sources of pollution include many common occupations (such as coal mining, welders).
Did you also know that cigarette smoke contributes to the toxicity of common air contaminants and remains the single largest cause of preventable death worldwide?
Therefore, understanding the impact of air pollution and cigarette smoke has been a crucial factor in implementing air quality guidelines and anti-tobacco campaigns. Despite this knowledge, we are seeing a surge in the use of emerging tobacco products such as e-cigarettes (“vape”), heat-not-burn products (IQOS) and hookah (includes e-hookah), particularly with young adults. However, the health effects of these products are almost completely unknown.
For this reason, one of the main programs of research for my laboratory is on tobacco-induced disease. We utilize in vitro and mouse inhalational models of tobacco smoke and other products to understand the pathogenesis of diseases such as chronic obstructive pulmonary disease (COPD). COPD is currently the 3rd leading cause of death world-wide.
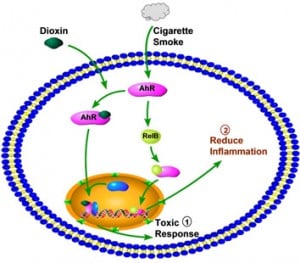
One of my research interests lay in identifying new molecular mechanisms involved in the pathogenesis of COPD, particularly ones that offers therapeutic potential or a novel susceptibility marker. To this end, we have been investigating the role the aryl hydrocarbon receptor (AhR) in the pathogenesis of smoke-induced lung disease. Our findings show that activation of the AhR by cigarette smoke suppresses inflammation and apoptosis in the lung. Using genetic and biochemical approaches, my research is focused on establishing that the AhR is a novel and important regulator of inflammation, oxidative stress and apoptosis. In conclusion, we wish to understand the role of the AhR in preventing morphological features of COPD in the lung and determine the molecular mechanism by which the AhR provides protection against the deleterious effects of tobacco smoke and other inhalational toxicants.
Biomedical Cannabis Research Program
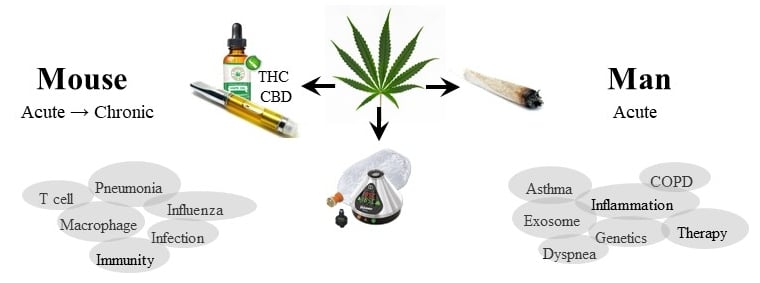
With my expertise in inhalation toxicology and mechanisms of disease pathogenesis, I have developed a new Cannabis Research Program fro my laboratory. Cannabis sativa indica- referred to as cannabis (marijuana) – is one of humanity’s oldest cultivated plants.
Cannabis has been used as a therapeutic agent for the management of pain, neurological conditions such as epilepsy and multiple sclerosis; inflammation; AIDS; cancer therapy and cancer-associated pain; anxiety; sleep; anorexia; convulsions; and respiratory conditions including asthma.
Working with clinicians and other scientists, we are working on an interdisciplinary program for biomedical cannabis research to explore the full potential of cannabis and cannabinoids in human health and disease. For this, we will have a state-of-the-art inhalation facility. This is important, as the most common way to consume cannabis is through inhalation (of smoke or vaporized cannabis/cannabinoids). With this, we will be able to deliver inhaled cannabis and cannabis-derived cannabinoids/novel drugs in a real-world scenario- to assess efficacy in disease models and understand the immune-medicated mechanisms involved in the potential therapeutic benefits of cannabis.
Pulmonary Fibrosis Research Program
Upwards of 45% of deaths in industrialized countries are due to fibrotic diseases of which renal, hepatic and pulmonary are the most common. Pulmonary fibrosis is a disease where the lungs becomes scarred and stiffened, leading to death from respiratory failure. The initiation of lung fibrosis is thought to be damage to the alveolar epithelium, leading to abnormal tissue repair typified by the accumulation of myofibroblasts. Myofibroblasts are α-smooth muscle actin (α-SMA)-expressing cells that secrete extracellular matrix (ECM) proteins under the direction of transforming growth factor-β (TGF-β). Pulmonary fibrosis shares many similarities with cancer, including fibroblastic foci, tissue hypoxia, aerobic glycolysis and increased TGF-β levels. Risk factors for pulmonary fibrosis include ionizing radiation and cigarette smoke.
There is no cure for pulmonary fibrosis and treatment options are few. A major impediment to the development of effective therapies is our limited understanding of the molecular pathways that drive fibrosis. Therefore, a focus of my overall research program is to identify novel cellular events leading to the development of fibrotic disease.
In the News

2026 RESP Research Day Poster and Oral Winners
Congratulations to all of our oral and poster presenter winners from the 2026 Respiratory Research Day

Sustaining Excellence Grants Keep High-Impact Research Moving Forward
Carolyn Baglole, Elizabeth Fixman, and Tania Janaudis-Ferreira received Sustaining Excellence Grants from the RI-MUHC.

Cannabis Vaping: Regulated Does Not Mean Safe
Carolyn Baglole discuss the SQDC’s decision to sell cannabis vape products and why “regulated” should not be confused with “safe”

Vaping, Smoking, and the Myth of a Safer Choice
Carolyn Baglole warns of rising youth smoking, stressing that neither cigarettes nor vaping are safe choices for health

Vaping Cannabis Could Harm Your Lungs
Research by Carolyn Baglole shows that cannabis vapour may contain harmful chemicals and affect lung cell function

Spring 2025 Student Awards
Congratulations to the 2025 recipients of FRQS and CIHR studentship and fellowship awards! We wish you much success!

2025 RESP Research Day Poster and Oral Winners
Congratulations to all of our oral and poster presenter winners from the 2025 Respiratory Research Day

Adolescent Vaping Linked to Increased Heart Disease Risk in Men
Two new studies by Carolyn Baglole examine how vaping during adolescence affects the lungs and heart.

DOM World Class Teams in TB and Pulmonary Fibrosis
Members of the RESP program are leading the Department of Medicine’s world class teams in Tuberculosis and pulmonary fibrosis.

Spring 2024 Student Awards
Congratulations to the 2024 recipients of FRQS and CIHR studentship and fellowship awards! We wish you much success!

2024 RESP Research Day Poster and Oral Winners
Congratulations to all of our oral and poster presenter winners from the 2024 Respiratory Research Day.

Smoking Bans and Vaping Restrictions: What the Science Really Says
Carolyn Baglole warns that vaping, once seen as safer than smoking, may cause lung damage, underscoring the need for strong regulation

CIHR Project Grant Results – Fall 2023
Congratulations to Carolyn Baglole and Andrea Benedetti, who were funded in the Fall 2023 CIHR Project Grant Competition!

Spring 2023 Student Awards
Congratulations to the 2023 recipients of FRQS and CIHR studentship and fellowship awards! We wish you much success!

Vaping can Cause Significant Harm to the Lungs
New research carried out in the lab of Carolyn Baglole, PhD, affirms that vaping can cause significant damage to the lungs.
Contact Information
Meakins-Christie Laboratories
RI-MUHC, Block E
Office EM2.2248
Lab E03.4374
1001 Decarie Blvd.
Montreal QC H4A 3J1
Canada
Tel: 514-934-1934
E-Mail: carolyn.baglole [at] mcgill.ca
Education & Training
BSc (Biology), U Prince Edward Island, 1993
MSc (Dev Biol), U Prince Edward Island, 1998
PhD (Pharmacol/ GISci), U Calgary, 2003
PDF/RAP (Lung Biol/Tox) U Rochester, 2010
Teaching
Biology of Disease: Environmental Toxicants, PATH 652